Published on September 22, 2022
Alzheimer’s Disease is a progressive, preventable brain disorder, NOT a normal part of aging. Share this research-based information to help lower the risk and incidence of Alzheimer’s with nutrients!
Key Points
- Alzheimer’s is a progressive brain disorder; more than 6.2 million Americans are living with Alzheimer’s, with more than 11 million American caregivers providing approximately 16 billion hours of unpaid care – valued at nearly 272 billion!
- There is a significant association between vitamin D deficiency and faster cognitive decline, as well as a 3-fold increase in the risk of Alzheimer’s disease among those with vitamin D deficiency and insufficiency
- Other nutrients that may help protect against Alzheimer’s disease and progression include magnesium, omega-3 fatty acids, B-vitamins, and probiotics
 According to the Alzheimer’s Foundation of America
According to the Alzheimer’s Foundation of America
- More than 6.2 million Americans are living with Alzheimer’s
- The number of Americans with Alzheimer’s is projected to surpass 13.8 million by 2060
- More than 11 million American caregivers provided approximately 16 billion hours of unpaid care – valued at nearly 272 billion!
Most importantly,
- Alzheimer’s is a progressive, preventable brain disorder, NOT a normal part of aging
The infographic below can be shared to help spread awareness about how specific nutrients can play a role in prevention and outcomes associated with Alzheimer’s Disease and dementia. Read below for a more detailed summary of research on how each nutrient can have a protective role on brain health and cognition, and can help decrease the risk of Alzheimer’s Disease and other forms of dementia.
Share the Research!
Low vitamin D associated with increased long-term risk of dementia and Alzheimer’s disease
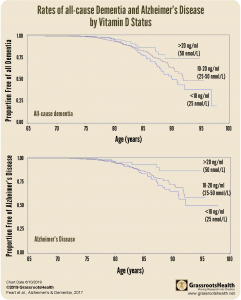 A 2017 study by Feart et al. looked at the association between vitamin D levels and risk of dementia in a French population consisting of 916 participants, aged 65 and older, whose measurements for vitamin D status and cognitive decline were tracked for 12 years. They found a significant association between vitamin D deficiency and faster cognitive decline, as well as a 3-fold increase in the risk of Alzheimer’s disease.
A 2017 study by Feart et al. looked at the association between vitamin D levels and risk of dementia in a French population consisting of 916 participants, aged 65 and older, whose measurements for vitamin D status and cognitive decline were tracked for 12 years. They found a significant association between vitamin D deficiency and faster cognitive decline, as well as a 3-fold increase in the risk of Alzheimer’s disease.
Associations appeared even stronger for the risk of [Alzheimer’s disease], with risks almost tripled in both deficient categories compared with sufficient concentrations.”
Vitamin D and the Risk of Dementia and Alzheimer’s Disease
A paper by Littlejohns et al. used data from 1,658 people in the US population-based Cardiovascular Health Study between 1992-1993 and 1999. Vitamin D samples were collected for all participants upon entry into the study. At the time of entry participants had a mean age of 74 years, were free from dementia, cardiovascular disease, and stroke and able to walk and get around on their own. They found that those with vitamin D levels < 10 ng/ml were 2.22 times more likely to get Alzheimer’s and 2.25 more likely to develop all-cause dementia than participants with vitamin D levels > 20 ng/ml.
Lower Risk for Alzheimer’s Disease and Dementia with Higher Vitamin D Levels
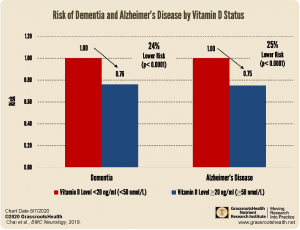 A 2019 meta-analysis by Chai et al. confirmed a significant association between higher levels of vitamin D (levels at or above 20 ng/ml or 50 nmol/L) and a decreased risk for both dementia and Alzheimer’s Disease. Data from a total of 21,784 participants in 11 different studies was included in the analysis for risk of dementia, while data from 14,618 participants in 6 different studies was analyzed for Alzheimer’s. The authors found an overall 24% lower risk of dementia and a 25% lower risk of Alzheimer’s for those whose vitamin D levels were at or above 20 ng/ml (50 nmol/L) compared to those with levels below 20 ng/ml.
A 2019 meta-analysis by Chai et al. confirmed a significant association between higher levels of vitamin D (levels at or above 20 ng/ml or 50 nmol/L) and a decreased risk for both dementia and Alzheimer’s Disease. Data from a total of 21,784 participants in 11 different studies was included in the analysis for risk of dementia, while data from 14,618 participants in 6 different studies was analyzed for Alzheimer’s. The authors found an overall 24% lower risk of dementia and a 25% lower risk of Alzheimer’s for those whose vitamin D levels were at or above 20 ng/ml (50 nmol/L) compared to those with levels below 20 ng/ml.
Magnesium Intake and Vitamin D Status May Help Prevent Cognitive Decline
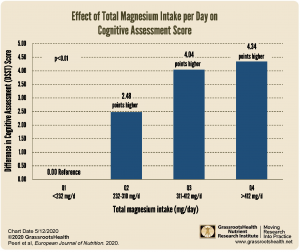 Using data from the National Health and Nutrition Survey (NHANES) 2011-2014, Peeri et al. studied the interaction between magnesium and vitamin D by assessing magnesium intake and serum vitamin D levels, and their association with cognitive decline in older adults. The analysis included 2466 participants ages 60 and older. The Digit Symbol Substitution Test (DSST), which measures cognitive performance by assessing executive function and processing speed, was used to identify and define the level of any existing cognitive impairment.
Using data from the National Health and Nutrition Survey (NHANES) 2011-2014, Peeri et al. studied the interaction between magnesium and vitamin D by assessing magnesium intake and serum vitamin D levels, and their association with cognitive decline in older adults. The analysis included 2466 participants ages 60 and older. The Digit Symbol Substitution Test (DSST), which measures cognitive performance by assessing executive function and processing speed, was used to identify and define the level of any existing cognitive impairment.
The authors found a significant association between magnesium intake and reduced odds of cognitive impairment for the third and highest quartiles of magnesium intake compared to the lowest (p trend <0.01), and similarly for the third and highest quartiles of vitamin D serum levels compared to the lowest (p trend=0.05). Compared to participants with the lowest magnesium intake amounts, participants with the highest intakes scored an average of 4.43 points higher on the DSST.
Cognitive Impairment Linked to Low Omega-3 Index
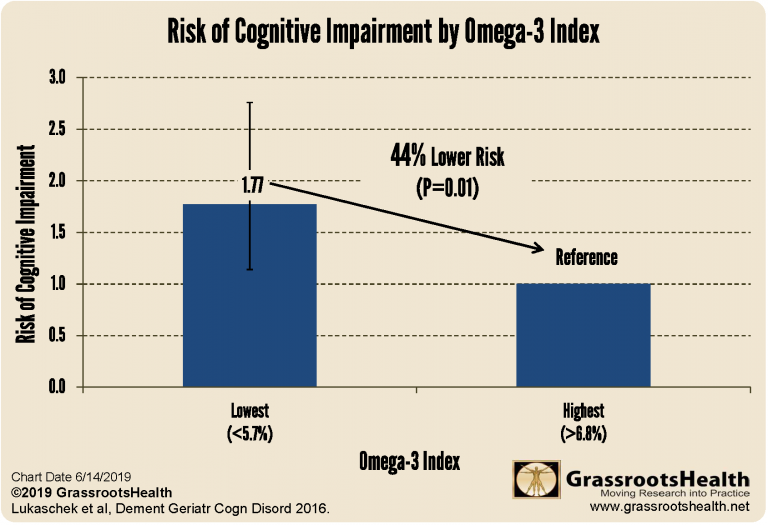 In 2016, results from a study by Lukaschek et al. assessing the association between Omega-3 Index, a biomarker of EPA and DHA status, and cognitive decline among older adults were published. This study included 720 participants aged 68 to 92 years old and assessed four cognitive domains: orientation, memory, attention, and language.
In 2016, results from a study by Lukaschek et al. assessing the association between Omega-3 Index, a biomarker of EPA and DHA status, and cognitive decline among older adults were published. This study included 720 participants aged 68 to 92 years old and assessed four cognitive domains: orientation, memory, attention, and language.
Participants with the highest Omega-3 Index levels (greater than 6.8%) had a 44% lower risk of cognitive impairment compared to participants with the lowest Omega-3 Index levels (less than 5.7%) (P=0.01).
Omega-3 Fatty Acid Status Improves the Protective Effects of B Vitamins on Cognition
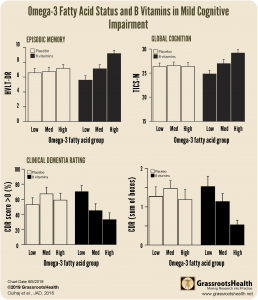 A 2016 randomized trial by Oulhaj et al. looked to see if omega-3 status has an influence on the effect of B vitamins on cognitive impairment. They enrolled 266 participants into the study, all of whom were at least 70 years of age and had mild cognitive impairment. Participants were randomized into either a high dose B vitamins (folic acid, B6, and B12) group or a placebo group for two years.
A 2016 randomized trial by Oulhaj et al. looked to see if omega-3 status has an influence on the effect of B vitamins on cognitive impairment. They enrolled 266 participants into the study, all of whom were at least 70 years of age and had mild cognitive impairment. Participants were randomized into either a high dose B vitamins (folic acid, B6, and B12) group or a placebo group for two years.
Outcomes were compared for those in the B vitamins group versus the placebo group based on baseline omega-3 status. Overall, significant benefits were found for those who had the higher baseline omega-3 fatty acid concentrations and who were in the B vitamin treatment group.
Those in the high omega-3 group who received B vitamins had
- improved episodic memory
- better global cognition scores
- lower ratings of dementia
With low omega-3 fatty acid concentrations, B vitamin treatment did not seem to slow cognitive decline in people with mild cognitive impairment. When omega-3 fatty acid levels were in the upper range of normal, the slowing effects of B vitamins on both brain atrophy and cognitive decline were enhanced.
This study supports previous evidence that the interaction of B vitamins and omega-3 fatty acids on brain atrophy and cognition results in the slowing down of the disease process in mild cognitive impairment.
Probiotics may help Improve C-Reactive Protein Levels in Alzheimer’s Patients
 A study by Walker et al. following over 12,000 individuals for 20 years found that those with the highest levels of CRP (4.69 mg/L or higher) had a 12% steeper cognitive decline compared to those with the lowest levels of CRP (≤1.04 mg/L).
A study by Walker et al. following over 12,000 individuals for 20 years found that those with the highest levels of CRP (4.69 mg/L or higher) had a 12% steeper cognitive decline compared to those with the lowest levels of CRP (≤1.04 mg/L).
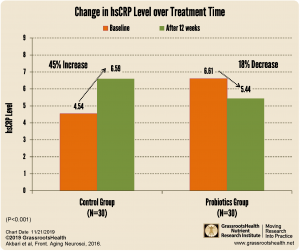
A 2016 randomized controlled trial by Akbari et al. followed 60 Alzheimer’s patients between the ages of 60 – 95 to determine whether probiotic supplementation had an effect on cognitive function and metabolic status, including CRP levels. For 12 weeks, half of the participants received a probiotic milk mix that contained Lactobacillus acidophilus, Lactobacillus casei, Bifidobacterium bifidum, and Lactobacillus fermentum (the probiotics group), while the other half received regular milk (the control group). Before and after measurements for mental state (which was evaluated with the mini-Mental State Examination, or MMSE test), hsCRP, and other markers for metabolism and inflammation were completed.
At the end of the 12 weeks, the probiotics group had an improvement in their MMSE score, while the control group had a worse MMSE score; the difference between the two groups was statistically significant. In addition, the probiotics group saw an 18% decrease in hsCRP levels, while the control group saw a 45% increase in hsCRP levels from the beginning of the 12 weeks to the end.
Make Sure Your Levels of the Above Are Supportive of Cognitive Health
 Having and maintaining healthy vitamin D and other nutrient levels can help improve your health now and for your future. Choose which to measure, such as your vitamin D, omega-3s, and essential minerals including magnesium and zinc, by creating your custom home test kit today. Add hs-CRP to measure your level of inflammation as well. Take steps to improve the status of each of these measurements to benefit your overall health. You can also track your own intakes, symptoms and results to see what works best for YOU.
Having and maintaining healthy vitamin D and other nutrient levels can help improve your health now and for your future. Choose which to measure, such as your vitamin D, omega-3s, and essential minerals including magnesium and zinc, by creating your custom home test kit today. Add hs-CRP to measure your level of inflammation as well. Take steps to improve the status of each of these measurements to benefit your overall health. You can also track your own intakes, symptoms and results to see what works best for YOU.
Enroll and test your levels today, learn what steps to take to improve your status of vitamin D (see below) and other nutrients and blood markers, and take action! By enrolling in the GrassrootsHealth projects, you are not only contributing valuable information to everyone, you are also gaining knowledge about how you could improve your own health through measuring and tracking your nutrient status, and educating yourself on how to improve it.






