Published on October 22, 2020
The difference between Omega-3 and Omega-6 fatty acids, how they affect human health, and how to balance them
In previous posts, we have reported on studies that demonstrate higher intake of omega-3 fatty acids help improve many health outcomes.
In fact, evidence suggests higher omega-3 intake may:
- Lower blood pressure and reduce blood triglyceride levels
- Slow the development of plaque in the arteries and development of heart disease
- Reduce the risk of heart attack, stroke and death
- Improve muscle stiffness, soreness, and range of motion recovery in athletes
- Improve mental health and prevent cognitive impairment
- Reduce the risk of non-melanoma skin cancer and breast cancer
- Improve immune response to infection
- Reduce levels of C-reactive protein and inflammation
Today, we will explain what omega-3 and omega-6 fatty acids are, how they affect human health, and how to balance them.
What Are Omega-3 and Omega-6 Fatty Acids?
Omega-3 and omega-6 fatty acids are two types of “essential” fatty acids, which means that we can’t make them in the body and must get them from our diet. While they differ chemically (in the length of their carbon chain and the location of double carbon bonds), they each have important health effects. They also provide a source of energy.
Both omega-3 and omega-6 fatty acids are important components of cell membranes that contribute to the structure, fluidity, flexibility, enzymatic activity and signaling between cells. It is through the roles that omega-3s and -6s play in cell membranes, particularly in inflammation, that their balance ultimately contributes to disease protection or susceptibility.
Omega-3 Fatty Acids
 The 3 most common types of omega-3s are:
The 3 most common types of omega-3s are:
Eicosapentaenoic acid (EPA): A 20-carbon fatty acid whose main function is to produce chemicals called eicosanoids, which help reduce inflammation.
Docosahexaenoic acid (DHA): A 22-carbon fatty acid, DHA makes up about 8% of brain weight and is extremely important for vision and for normal brain growth and development during pregnancy and infancy.
Alpha-linolenic acid (ALA): An 18-carbon fatty acid, ALA is mainly used by the body for energy. ALA can be converted into EPA and DHA, although it is not an efficient process.
Omega-3s are found in the diet in many forms. Fatty fish such as salmon, mackerel, tuna, herring and sardines are good sources of EPA and DHA. Nuts and seeds (such as flaxseed, chia seeds and walnuts) as well as plant oils (such as flaxseed and canola oil) contain ALA.
Omega-6 Fatty Acids
 Omega-6 fatty acids provide an important source of energy for the body. The most common omega-6 fat is linoleic acid (LA), which can be converted into longer omega-6 fats such as arachidonic acid (AA).
Omega-6 fatty acids provide an important source of energy for the body. The most common omega-6 fat is linoleic acid (LA), which can be converted into longer omega-6 fats such as arachidonic acid (AA).
Linoleic acid (LA): An 18-carbon fatty acid, LA has a direct role in maintaining the integrity of the water permeability barrier of the skin. LA also helps lower blood cholesterol levels. It is estimated that LA accounts for approximately 90% of dietary omega-6 fatty acids.
Arachidonic acid (AA): A 20-carbon fatty acid, AA is used to form chemical messengers important for muscle function, blood clotting, and inducing inflammation.
Omega-6 fats are found in large amounts in refined vegetable oils and foods cooked in vegetable oils which are abundant in the Western diet. Nuts, seeds, meat and dairy also contain omega-6 fatty acids.
What Do They Do?
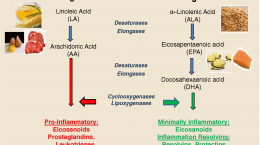
Omega-3s and omega-6s in the cell membrane play different roles in inflammation, as illustrated in the diagram below. Omega-6s (such as AA) are essential for initiating and sustaining the inflammatory response – a physiologic function necessary for healing from injuries and infection. Omega-3s (such as DHA and EPA) are anti-inflammatory and promote the resolution of the inflammatory process.
Pro-inflammatory eicosanoids produced from omega-6s are important chemicals in the immune system. However, when too many of them are produced, they can suppress the immune system, promote blood clotting and increase inflammation and inflammatory disease. Unfortunately, a majority of the population consumes too many omega-6s and too few omega-3s, which leads to an abundance of omega-6s in the cell membrane.
The Role of Omegas in Inflammation and Health
Increased omega-3 fatty acid intake has been associated with a reduced risk of heart disease, diabetes, cancer and death. Chronic inflammation is a key contributor to the development of all of these conditions.
Omega-3 fatty acids are consistently linked with improved heart health outcomes. Observational studies demonstrate a protective effect of omega-3s against heart disease through several mechanisms including reducing blood triglycerides, blood pressure, blood clotting, growth of atherosclerotic plaques and anti-inflammatory effects.
Several studies have also found increased levels of pro-inflammatory activity among cancerous cells. Inflammation promotes an environment in which cancer can develop and grow and is recognized as one of the drivers. Increasing anti-inflammatory dietary factors are a potential method for mitigating inflammation and reducing the risk of cancer development and progression. Further, it is thought that increasing omega-3s in the cell membrane may help disrupt the signals, called an oncogenic protein, that lead to cancer development.
So how might increasing omega-3s help prevent chronic disease? Reducing inflammation reduces the positive feedback it has on atherosclerotic plaque and cancer development and progression. Counteracting the influence of pro-inflammatory omega-6s and their production of inflammatory signals (eicosanoids, prostaglandins, leukotrienes and thromboxanes) can be achieved through increasing omega-3s and the production of anti-inflammatory signals (resolvins and protectins), reducing inflammation.
How Much Omega-3 Do You Need?
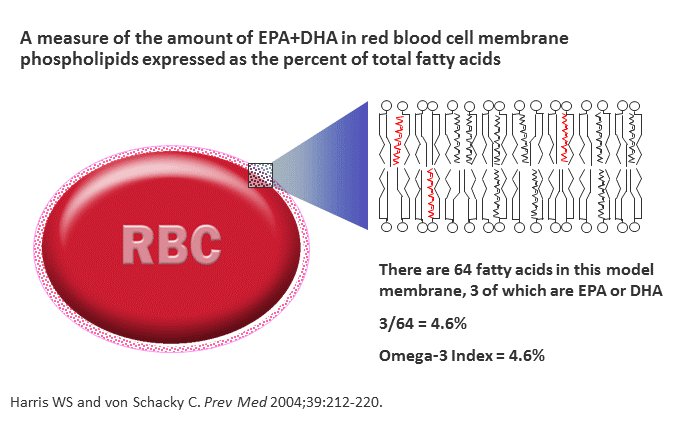
Increasing omega-3 fatty acids, in the diet or through supplementation, is recommended to balance the effects of omega-6s. Increasing omega-3 fatty acid intake likewise increases the omega-3 content of cell membranes including red blood cells, immune cells, heart muscle and other types throughout the body, and can contribute to reduced risk of disease and death.
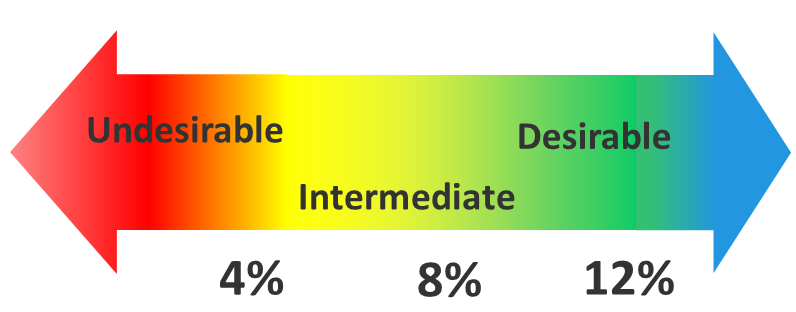
The Omega-3 Index is a measurement of the amount of the EPA and DHA in red blood cell (RBC) membranes. Studies have shown that an Omega-3 Index at or above 8% is optimal and less than 4% is deficient, particularly for cardiovascular disease.
GrassrootsHealth published a paper that assessed the EPA+DHA intake requirement to achieve an Omega-3 Index of 8% or higher, and using YOUR data found: ~1,300 mg/day of EPA+DHA was needed for 50% of the population and ~1,900 mg/day was needed for 90% of the population to achieve an Omega-3 Index of 8%.
Know Your Omega-3 Status
GrassrootsHealth offers several testing options to help measure the status of omega-3 and omega-6 fatty acids – the Omega-3 Index, AA:EPA Ratio, and Omega-6:Omega-3 Ratio. Learn more about these tests and the differences between them here. More information on how to improve these test results can be found here.
What is Your Level of Inflammation? Are You Getting Enough Omega-3s and Other Nutrients?
Join the Breast Cancer Prevention Study to find out! Using the GrassrootsHealth Custom Kit Builder, you can create a test kit that measures the status of nutrients important to the regulation of inflammation (such as vitamin D, omega-3s, and magnesium), as well as your CRP level. Click here to build and order your test kit today – measure your status and take the steps necessary to improve them if needed; make an impact on your health today and for your future! When you know what your levels are, you can determine next steps to take and how much supplementation may be needed if you are not at your target levels.
Concerned specifically about your immune health? See if your immune system might be needing more vitamin D and other immune boosting nutrients by enrolling in the Immune Boost Project with the Full Immune Boost Panel (which includes tests for vitamin D, Omega-3 Index, magnesium, zinc, selenium, copper, and hsCRP).
What are Your Levels?
Through GrassrootsHealth Nutrient Research Institute, you can test your vitamin D, essential elements magnesium, copper, zinc and selenium, toxins such as lead, mercury and cadmium, as well as your omega-3 levels, inflammation levels and thyroid stimulating hormone (TSH) level. Find out your levels today! Log on to the test selection page (click the link below) to get your tests and see for yourself if your levels can be improved.
Make sure you track your results before and after, about every 6 months!
How can I track my nutrient intake and levels over time?
To help you track your supplement use and nutrient levels, GrassrootsHealth has created the Personal Health Nutrient Decision System called
For each specific supplement, you can track what days you take it, how much, and many other details. This will help you know your true supplemental intake and what patterns of use work for you to reach and maintain optimum nutrient levels. Check it out today!