Published on December 14, 2020
If something so devastating can be so easily prevented, why is it still a problem?
 GrassrootsHealth occasionally receives an email from a parent or grandparent struggling with the consequences of infantile rickets, often mis-diagnosed as a case of child abuse. At the same time, news outlets across the globe have been reporting a resurgence of rickets over the past several years. The causes being cited are the increased popularity of breast feeding and failure of doctors to prescribe vitamin D supplements to infants. The issue is disproportionately on the rise in (although not limited to) dark-skinned children who cannot make enough vitamin D from their limited sun exposure.
GrassrootsHealth occasionally receives an email from a parent or grandparent struggling with the consequences of infantile rickets, often mis-diagnosed as a case of child abuse. At the same time, news outlets across the globe have been reporting a resurgence of rickets over the past several years. The causes being cited are the increased popularity of breast feeding and failure of doctors to prescribe vitamin D supplements to infants. The issue is disproportionately on the rise in (although not limited to) dark-skinned children who cannot make enough vitamin D from their limited sun exposure.
There are no national rates for rickets in the US because it is not a reportable public health disease, and there are no surveillance systems that capture nation-wide information about it. In the UK, however, the Daily Mail cited 833 hospital admissions for rickets in 2012, more than four times the amount 10 years earlier.
What is rickets?
 Rickets is a disorder characterized by softening and weakening of the bones resulting from a lack of vitamin D, calcium, or phosphate. Symptoms of rickets include bone pain or tenderness, decreased muscle tone, dental deformities, impaired growth, increased bone fractures, muscle cramps, short stature, and skeletal deformities such as the characteristic bowlegs.
Rickets is a disorder characterized by softening and weakening of the bones resulting from a lack of vitamin D, calcium, or phosphate. Symptoms of rickets include bone pain or tenderness, decreased muscle tone, dental deformities, impaired growth, increased bone fractures, muscle cramps, short stature, and skeletal deformities such as the characteristic bowlegs.
After being diagnosed with rickets, treatment is to replace the vitamin D, calcium and phosphorus that is lacking. If done during childhood, treatment usually eradicates all symptoms. Vitamin D levels of 20 ng/ml or higher will prevent most cases of rickets, so children diagnosed with rickets are generally severely vitamin D deficient.
Background on rickets
Rickets was a common childhood ailment prior to and throughout the Industrial Revolution, up until the 1940s, affecting thousands of children annually. In the 1920s and 30s the cause of rickets was determined and public health practices, including the fortification of milk with vitamin D and recommended use of cod liver oil, started to gain favor. Since that time both infant formula and milk have been fortified with vitamin D and the disease was almost eradicated.
Three prevalent positions spell trouble for infants
 With the resurgence of breast feeding, more babies are off infant formula and are not getting vitamin D supplementation. This would be fine if the mother had a daily vitamin D intake (through sun exposure, food, or supplements) that resulted in 25(OH)D concentration of 40 ng/ml or higher. But most doctors do not know to tell breast feeding mothers this information, nor do they prescribe vitamin D supplementation to infants. In fact,
With the resurgence of breast feeding, more babies are off infant formula and are not getting vitamin D supplementation. This would be fine if the mother had a daily vitamin D intake (through sun exposure, food, or supplements) that resulted in 25(OH)D concentration of 40 ng/ml or higher. But most doctors do not know to tell breast feeding mothers this information, nor do they prescribe vitamin D supplementation to infants. In fact,
- the average US adult has a vitamin D blood level of about 28 ng/ml or 70 nmol/L (NHANES)
- AND… doctors are not recommending supplementation for infants or their mothers
- AND…. doctors are recommending that mothers and their infants stay out of the sun, cover up, or use sunscreen
The result is that most mothers and their babies are not getting enough vitamin D and rickets is re-emerging.
Lack of vitamin D supplementation in infants
Our panel of scientists recommend infants (< 1 year) take 400 IU vitamin D daily starting a few days after delivery. The easiest way for an infant to receive supplementation is by using drops (Google: ‘vitamin D drops’).
Carol Wagner, MD studied vitamin D in infants and found that with 400 IU/day the mean vitamin D level in her study group increased from 16 ng/ml (at 1 month) to 43 ng/ml (at 4 months) and 42 ng/ml (at 7 months).
Failure to improve despite updated recommendations
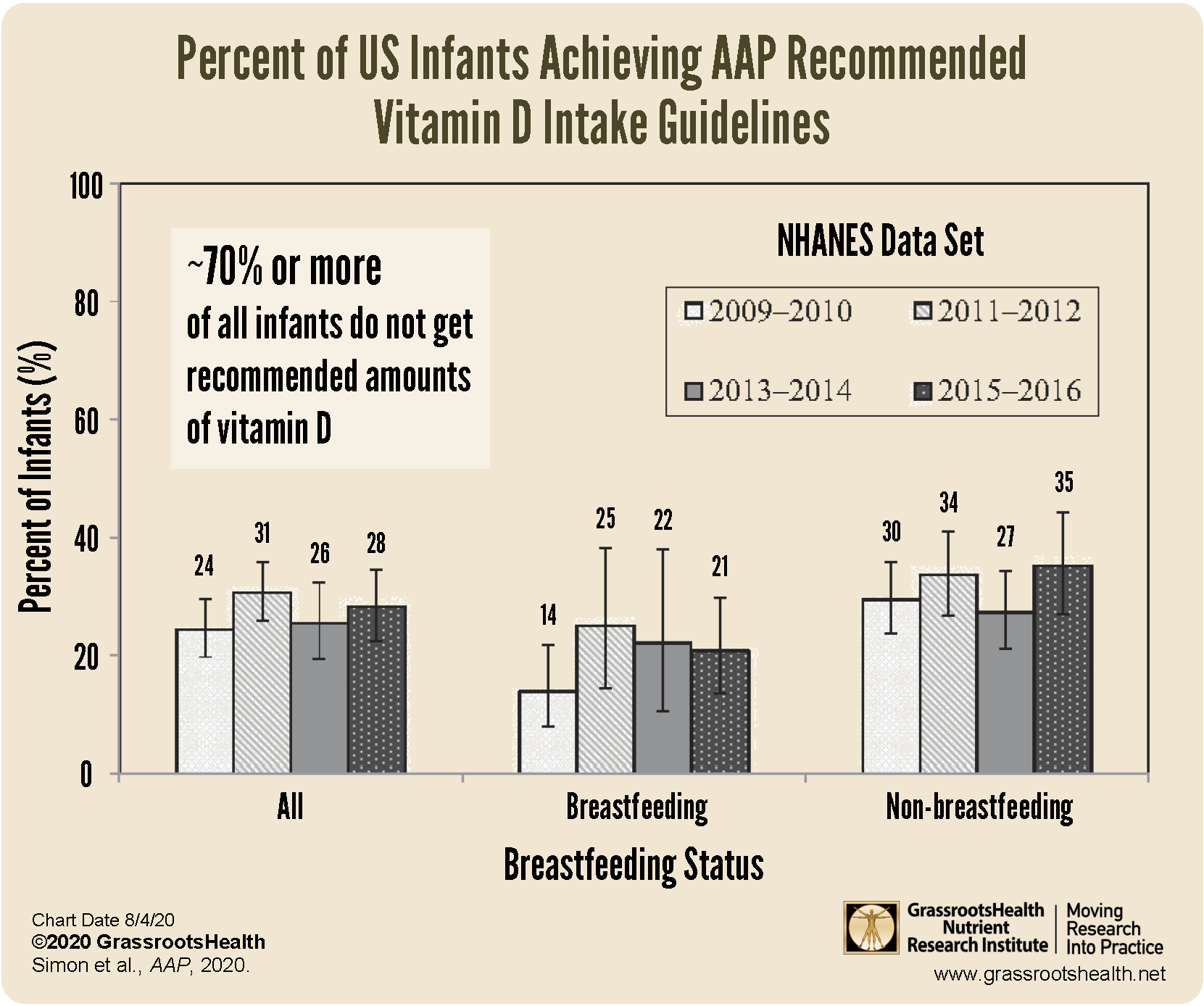
A 2020 review published by Simon and Ahrens looked at NHANES vitamin D intake amounts among US infants for the years 2009 – 2016. The authors found no increase in the percent of infants achieving the recommended vitamin D intake since the American Academy of Pediatrics revised their guidelines in 2008. In fact, only 27% of all infants met vitamin D intake guidelines, with breastfeeding infants being less likely to meet the guidelines than non-breastfeeding infants.
How to get vitamin D in breast milk
 Another way to provide vitamin D for an infant is to ensure that there is enough vitamin D in the breast milk. This is possible and has been demonstrated by Dr. Wagner in a lactation study that found women who have vitamin D levels of at least 40 ng/ml can transfer vitamin D to their babies. She found that 6400 IU/day was necessary for the women to stay replete in vitamin D and that this would be equivalent to babies getting a 400 IU/day supplement.
Another way to provide vitamin D for an infant is to ensure that there is enough vitamin D in the breast milk. This is possible and has been demonstrated by Dr. Wagner in a lactation study that found women who have vitamin D levels of at least 40 ng/ml can transfer vitamin D to their babies. She found that 6400 IU/day was necessary for the women to stay replete in vitamin D and that this would be equivalent to babies getting a 400 IU/day supplement.
For more on this, please watch Dr. Wagner’s presentation on Vitamin D and Public Health: Integrating sunshine, supplement, and measurement for optimal health. Information from this lactation study is included toward the end (minutes 34:30 -> end).
In his blog Vitamin D and the nursing mother, Dr. Robert Heaney ends with a call to action that all mothers supplement with 5,000 – 6,000 IU/daily because doing so would provide the needed benefit for both the mother and baby, naturally. He also makes a very important point that supplementation needs to be daily:
“There is one important proviso for nursing mothers concerning the needed intake. Those who live in North America and have to rely on supplements should be certain that they take their supplements every day. While for other purposes it is possible to take vitamin D intermittently (e.g., once a week), that doesn’t work for putting vitamin D into human milk. The residence time of vitamin D in the blood is so short that, if the mother stops taking her vitamin D supplement for a day or two, vitamin D in her milk will be low (or absent altogether) on the days she skips.”
Rickets or Child Abuse?
 Because rickets had been so rare, many doctors practicing just ten years ago had never seen a case in person and today many still don’t recognize it when they do see it. There have been several cases where children have been pulled away from their families by child protective services (CPS) due to undiagnosed rickets. The children are brought into a medical facility for some treatment (sickness, disease) and broken bones or signs of healing bones are found and presumed to be a result of abuse. At this point CPS is contacted and sometimes the children taken away.
Because rickets had been so rare, many doctors practicing just ten years ago had never seen a case in person and today many still don’t recognize it when they do see it. There have been several cases where children have been pulled away from their families by child protective services (CPS) due to undiagnosed rickets. The children are brought into a medical facility for some treatment (sickness, disease) and broken bones or signs of healing bones are found and presumed to be a result of abuse. At this point CPS is contacted and sometimes the children taken away.
Dr. Wagner consulted on such a case where twin 6 month old boys (and their 3 older brothers) were removed from their loving home because of a broken rib and threat of child abuse. The mother was severely vitamin D deficient during pregnancy, and after, and solely breast fed the twins. Vitamin D tests for the twins showed their levels to be < 10 ng/ml. After much work by Wagner and their lawyer the children are now back with their family – and hopefully the whole family is getting sun and supplementation.
Ensure Vitamin D Levels of 40-60 ng/ml (100-150 nmol/L) for You, Your Children, Loved Ones
Correcting a vitamin D deficiency at any age and any time of life decrease potential disease severity and improve outcomes! Test your vitamin D level today, learn what steps to take to improve your level, and take action to achieve and maintain a vitamin D level of 40-60 ng/ml (100-150 nmol/L).
Using the GrassrootsHealth Custom Kit Builder, you can create a test kit that measures your status of vitamin D and other important nutrients (such as omega-3s, zinc and magnesium), as well as your CRP level to measure inflammation. Click here to build and order your test kit today – measure your status and take the steps necessary to improve them if needed; make an impact on your health today and for your future! When you know what your levels are, you can determine next steps to take and how much supplementation may be needed if you are not at your target levels.
Enroll now with the Full Immune Boost Panel (which includes tests for vitamin D, Omega-3 Index, magnesium, zinc, selenium, copper, and hsCRP), and get 10% off when you use coupon code BoostTen at checkout.