Published on June 29, 2020
The liver, which is the body’s largest internal organ, has many important functions, including the production of proteins and bile, metabolism of nutrients for energy, and removing hazardous toxins from the body. When the liver becomes damaged, taxed, or diseased, the level of liver enzymes within the blood becomes elevated. These enzymes, which include alanine transaminase (ALT) and aspartate transaminase (AST), are often used to identify a potential liver disease, such as hepatitis (swelling of the liver), cirrhosis, nonalcoholic fatty liver disease, metabolic syndrome, and alcoholic liver disease. The liver is also responsible for producing certain chemicals in the body that can be used as indicators of health, such as homocysteine and C-reactive protein, both of which have been associated with a greater risk of cardiovascular disease when elevated.
Could Vitamin D be related to Liver Health?
 In addition to the above, the liver is also responsible for converting much of the vitamin D3 from the blood into 25(OH)D; it has therefore been speculated that liver disease and poor liver function may contribute to low 25(OH)D levels, or a level that does not respond well to supplementation. However, there also seems to be a reverse effect – where low levels of vitamin D potentially hinder the function and health of the liver.
In addition to the above, the liver is also responsible for converting much of the vitamin D3 from the blood into 25(OH)D; it has therefore been speculated that liver disease and poor liver function may contribute to low 25(OH)D levels, or a level that does not respond well to supplementation. However, there also seems to be a reverse effect – where low levels of vitamin D potentially hinder the function and health of the liver.
A randomized double-blind placebo controlled clinical trial conducted by Al-Bayyari et al. investigated whether improving vitamin D serum levels had a beneficial effect on liver function, as well as other markers of inflammation, kidney function, and cardiovascular health. The study consisted of 100 women of reproductive age (18 to 49 years), who were overweight (with a BMI between 25-29.9 kg/m2) and who presented with vitamin D deficiency (<20 ng/ml). All women were also free from any existing chronic diseases.
50 women received 50,000 IU of vitamin D every week for 2 months, while the other 50 women received a placebo. Blood measurements for vitamin D, total homocysteine (tHyc), C-reactive protein (CRP), the liver enzymes alanine aminotransferase (ALT) and aspartate aminotransferase (AST), and urea and creatinine for kidney function were taken before and after intervention.
What did this study find?
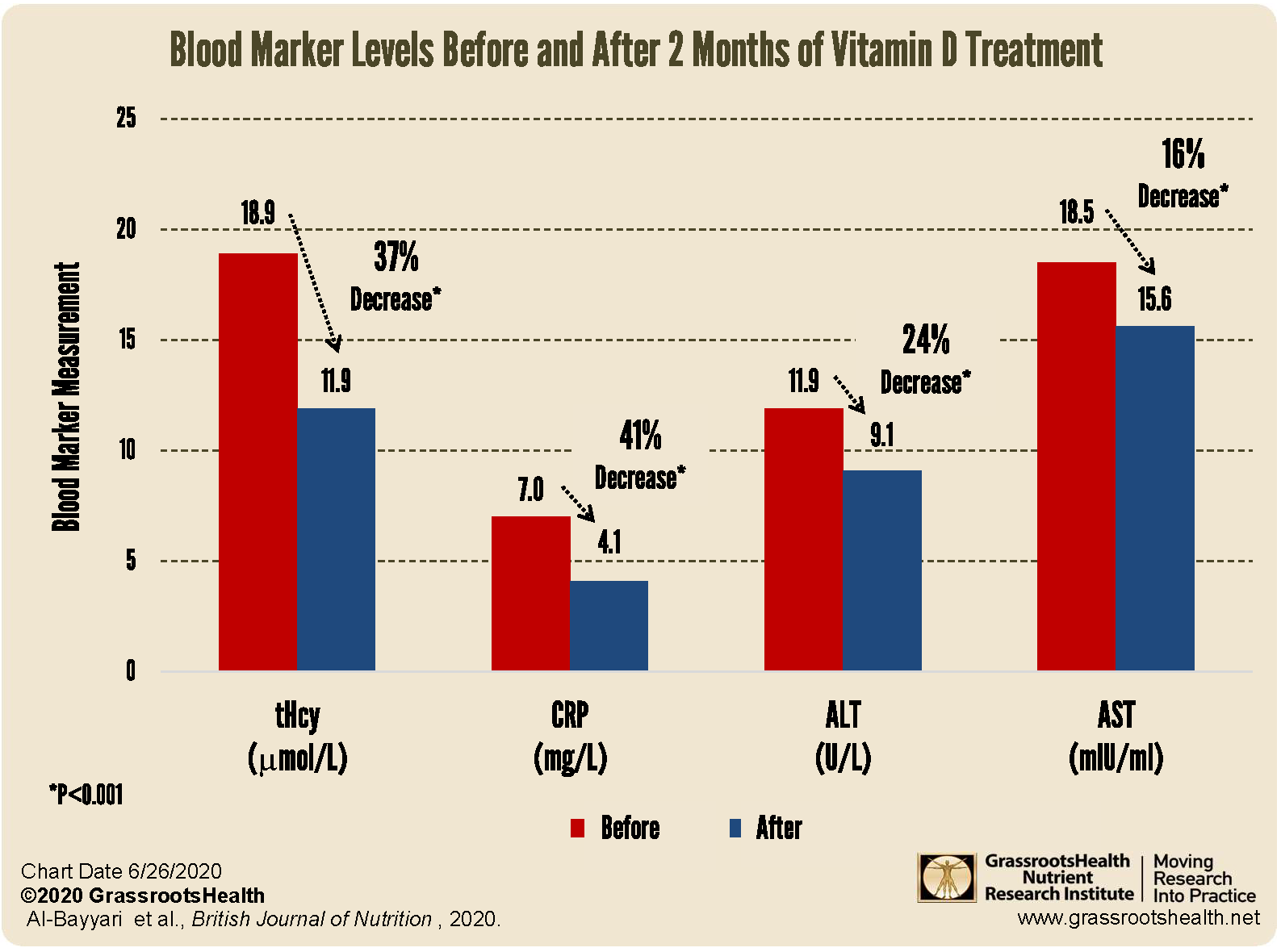
The average baseline BMI for all subjects was 27.1 kg/m2, with an average tHcy of 18.4 umol/L and average vitamin D level of 8.5 ng/ml. While the placebo group had no statistically significant differences in baseline and post-intervention measurements, those in the vitamin D supplementation group saw statistically significant differences (p<0.001) in the before and after levels with decreases of tHcy, CRP, ALT and AST (shown in the chart above), and increases in vitamin D, urea, and creatinine.
The Relationship between Vitamin D & CRP
Inflammation is a known contributing factor to many diseases and is often measured by CRP, one of the best markers of inflammation, especially for inflammation caused by bacterial infection or tissue damage. Studies have associated vitamin D with lower levels of inflammation and CRP, in diseases such as in cardiovascular disease, psychiatric disorders, and diabetes. Research is also showing a relationship between higher CRP levels and an increased risk for and severity of COVID-19. This, among the slew of research showing increased risk and severity of COVID 19 with vitamin D deficiency, adds to the evidence of the importance of vitamin D for a healthy immune and inflammatory response, especially now.
Test your vitamin D and CRP levels today!
Are You Getting Enough Vitamin D?
Do you know what your vitamin D level is? Be sure to test today to find out, and take steps to keep it within a target of 40-60 ng/ml or 100-150 nmol/L! Give your immune system the nutrients it needs to support a healthy you and protect yourself from unnecessary diseases.
Through GrassrootsHealth Nutrient Research Institute, you can also test your essential elements magnesium, copper, zinc and selenium, toxins such as lead, mercury and cadmium, as well as your omega-3 levels, inflammation levels and thyroid stimulating hormone (TSH) level. Find out your levels today! Log on to the test selection page (click the link below) to get your tests and see for yourself if your levels can be improved.
Make sure you track your results before and after, about every 6 months!
How can I track my nutrient intake and levels over time?
To help you track your supplement use and nutrient levels, GrassrootsHealth has created the Personal Health Nutrient Decision System called
For each specific supplement, you can track what days you take it, how much, and many other details. This will help you know your true supplemental intake and what patterns of use work for you to reach and maintain optimum nutrient levels. Check it out today!