Published on January 26, 2022
How the ongoing vitamin D debate in the scientific community may be affecting decisions about vitamin D for you and your loved ones
Key Points
- In the medical science world, data from randomized controlled trials (RCTs) are considered the “gold-standard” evidence, as these types of studies are designed specifically to determine the cause and effect relationship of an intervention (such as a drug) on a primary outcome. Unfortunately, these costly studies can be difficult to optimize and interpret for nutrients, especially vitamin D.
- Many studies, including case-control studies, cohort studies, cross-sectional studies, and even some RCTs, have shown that vitamin D can benefit our immune, cardiovascular, cognitive, and overall health, and reduces the risk of many diseases
- It is essential to consider the “Totality of Evidence” when making decisions about vitamin D for health

We know, beyond a doubt, that vitamin D is essential for our health. Many studies have shown that vitamin D can benefit our immune, cardiovascular, cognitive, and overall health, and reduces the risk of many diseases. Unfortunately, due to the complicated nature of nutrient research, there remains scientific debate about what absolute proof exists to support the need for vitamin D supplementation, in what amounts, and what specific health outcomes are affected by varying levels of vitamin D.
The Traditional Evidence Pyramid in Medical Research
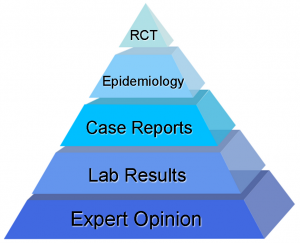 Dr. Reinhold Vieth spoke of the Evidence Pyramid when relating vitamin D research to multiple sclerosis outcomes.
Dr. Reinhold Vieth spoke of the Evidence Pyramid when relating vitamin D research to multiple sclerosis outcomes.
At the wide, low end of the evidence pyramid is what was once known as expert opinion, i.e. what the esteemed professor says. This is a wide base because there are a lot of experts and everyone has an opinion, however, opinion is not proof of anything. Next is evidence from the laboratory, be it cellular biology or animal research, which generates scientific data relatively easily but can be difficult to translate to clinical practice. Higher on the pyramid still are case histories or case reports that present the experience of individual patients, which can lack context.
Still higher up the pyramid is the important field of epidemiology, the study of disease in populations. Epidemiology is powerful; it put anti-smoking and seatbelt use into public policy. It demonstrates relationships, but is not absolute proof that a specific variable can be the cause of a certain outcome. In a court of law, epidemiology would still be called circumstantial evidence.
At the very top of the Evidence Pyramid are the randomized double-blind, placebo-controlled trials (RCTs). In the medical science world, data from RCTs are considered the “gold-standard,” as these types of studies are designed specifically to determine the cause and effect relationship of an intervention (such as a drug) on a primary outcome. Unfortunately, these costly studies can be difficult to optimize and interpret for nutrients, especially vitamin D. Dr. Robert Heaney reviewed this issue in detail and created specific guidelines that must be followed for findings from vitamin D RCTs to be considered accurate. This topic will be covered more in another upcoming post.
What to do About Vitamin D? Consider “The Totality of Evidence”
As Dr. Vieth quoted, while vitamin D RCTs may not ever be a reality for many disease outcomes, “Nonetheless, like many things in life, we need to decide our actions without perfect knowledge.”
Instead, perhaps we should consider “The Totality of Evidence.” The following is a diagram from the FLCCC Alliance – COVID-19 Management Protocol overview document, and it is an excellent illustration of the totality of evidence to consider when making health decisions (for nutrients, consider replacing “Pharmacology” with “Nutritional Pharmacology” and adding “Physiology” to “Basic Science”).
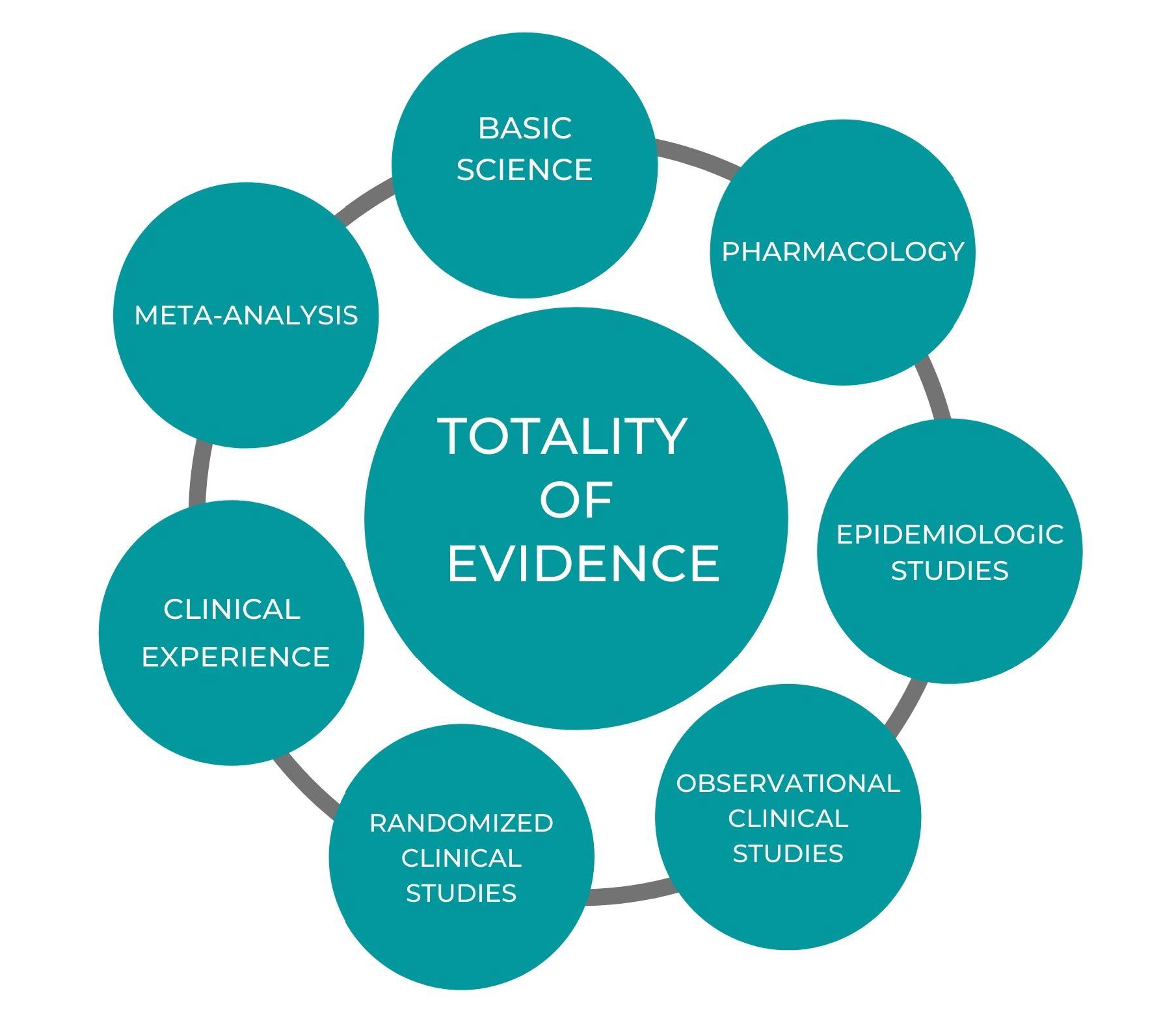
The diagram can be broken down as follows for vitamin D:
Basic Science/Physiology – We know that most cells and tissues in the body have vitamin D receptors and a need for vitamin D. The body makes vitamin D upon exposure to UVB radiation, in amounts such that one minimal erythema dose is equivalent to roughly 10,000 – 25,000 IU of supplemental vitamin D. If given the chance and under the right circumstances, the body produces enough vitamin D from sunshine to reach levels of 40-60 ng/ml (100-150 nmol/L), which are levels found among individuals with high sun exposure, such as hunter-gatherer tribes in Africa and lifeguards in Southern California. In other words, vitamin D levels of 40-60 ng/ml (100-150 nmol/L) are achieved naturally with proper sun or UVB exposure.
Nutritional Pharmacology – This can be considered as the specific biochemical or physiological effects that vitamin D has on cells, tissues, and the whole individual – or HOW vitamin D affects us. Mechanistic studies (which are designed to identify how something works to produce a certain effect, or to determine a mechanism of action) have demonstrated how vitamin D works within the cells, tissues, organs, and the body as a whole to directly influence health and the development or regression of many skeletal and non-skeletal diseases. Examples of this type of evidence include how vitamin D influences changes in genetic expression and how immune cells rely on vitamin D for specific functions.
Clinical Experience – What differences are noticed by care providers when a vitamin D deficiency is corrected or a supplementation routine is started and maintained over time? Doctors and other health care providers who are aware of vitamin D deficiency and who regularly test and supplement to achieve target vitamin D levels are able to observe the changes within their patient population, and therefore build a hands-on relationship with vitamin D. Such practice over time is extremely meaningful and can demonstrate safety and overall effects of its use in clinical practice. This is real-world data in practice!
Observational Clinical Studies – There are many clinical studies that have demonstrated significant benefits of vitamin D for clinical populations. An example is the study implemented at the Medical University of South Carolina in collaboration with GrassrootsHealth which demonstrated the effects of a new vitamin D program on prenatal outcomes. This project launched a new standard of care for prenatal patients that included vitamin D testing and personalized supplementation to achieve a minimum vitamin D level of 40 ng/ml (100 nmol/L), and it demonstrated both the effectiveness and safety of vitamin D testing, supplementation, and education on specific health outcomes for pregnant women.
Epidemiologic Studies – There are many types of epidemiologic studies, including cohort studies, case-control studies, cross-sectional studies, and ecologic studies that have demonstrated a strong link between vitamin D and specific health outcomes. As described above, these studies help reveal relationships and patterns within a population, such as the incidence, prevalence, or risk of a certain disease when specific variables are involved. An example of an ecological study, which does not use individual’s data, is the discovery made by the Garland brothers that cancer rates tended to be higher at higher latitudes where there is less UVB and therefore less vitamin D produced year-round.
Cohort studies, like our GrassrootsHealth D*action Study, follow a group of people over time and seeks to determine the association between a particular exposure (something people are doing, eating or being exposed to as part of their daily lives), and an outcome (such as developing cancer), while adjusting for other risk factors that could bias the results (such as age or BMI). These types of studies rely on data from a collection of individuals, and since exposures and outcomes are collected in chronological order, cohort studies, similar to RCTs, can distinguish between cause and effect, as explained in further detail here.
Randomized Clinical Studies – Several RCTs on vitamin D have shown promise, such as those on breast cancer, however, the design of such studies should follow specific guidelines in order for the findings to be considered exceptionally valid. This will be discussed in detail in another upcoming post.
Meta-Analysis – These reviews take a look at a combined set of research on a specific outcome, such as those looking at the effect of vitamin D levels and supplementation on COVID-19 infection risk, severity, and mortality, and can be a very powerful tool for making overall conclusions about the effect of vitamin D on health.
What information are you relying on to make your health decisions with vitamin D?
Vitamin D is an Easily Modifiable Factor to Help Improve Disease Outcomes
 Having and maintaining healthy vitamin D levels and other nutrient levels can help improve your health now and for your future. Choose which additional nutrients to measure, such as your omega-3s and essential minerals including magnesium and zinc, by creating your custom home test kit today. Take steps to improve the status of each of these measurements to benefit your overall health. You can also track your own intakes, symptoms and results to see what works best for YOU.
Having and maintaining healthy vitamin D levels and other nutrient levels can help improve your health now and for your future. Choose which additional nutrients to measure, such as your omega-3s and essential minerals including magnesium and zinc, by creating your custom home test kit today. Take steps to improve the status of each of these measurements to benefit your overall health. You can also track your own intakes, symptoms and results to see what works best for YOU.
Enroll and test your levels today, learn what steps to take to improve your status of vitamin D (see below) and other nutrients and blood markers, and take action! By enrolling in the GrassrootsHealth projects, you are not only contributing valuable information to everyone, you are also gaining knowledge about how you could improve your own health through measuring and tracking your nutrient status, and educating yourself on how to improve it.