Published on April 22, 2019
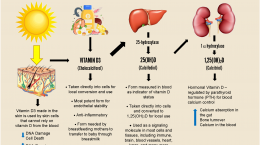
Vitamin D has many uses in the body and comes from many sources. In previous blogs, we have discussed how to increase vitamin D levels by getting vitamin D from food, supplements, and sun. We recently covered the association between vitamin D in the blood and vitamin D levels in fat. Today, we will focus on the conversion and use of vitamin D, as illustrated in the diagram below by Heaney and Armas.
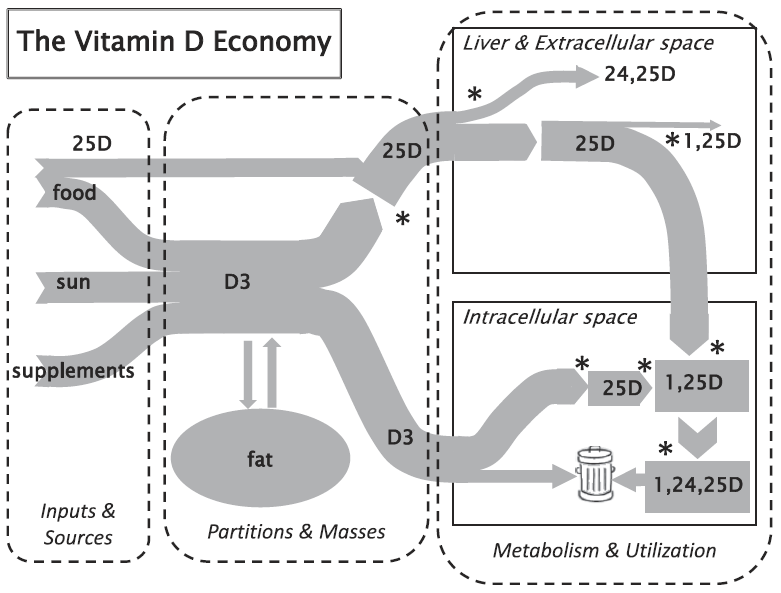
* points where hydroxylation reactions occur.
Vitamin D3 to 25(OH) Vitamin D
While it has been shown that some vitamin D3, the form that we take as a supplement and make in our skin, is absorbed directly into and utilized within the cells themselves, the majority of vitamin D3 goes to the liver for its first conversion process, 25-hydroxylation. This process converts vitamin D3 into 25-hydroxyvitamin D (or 25(OH)D), which is this form of vitamin D that is measured in the blood as an indication of an individual’s overall vitamin D status.
A very small amount of 25(OH)D is ingested directly from animal foods, but the majority of vitamin D in the body begins as vitamin D3.
1,25(OH)2D – the “Active” Form of Vitamin D
Conversion of 25(OH)D into what is commonly known as the “active” form of vitamin D, 1,25(OH)2D (or 1,25D), is done mostly in the kidneys as part of vitamin D’s function within the endocrine system. In this case, the process is highly regulated by the parathyroid through what is known as a “negative feedback loop.”
1,25D is the main regulator of calcium absorption in the intestines – when calcium levels are low, the parathyroid initiates an increase in the rate of conversion of 25(OH)D to 1,25D, which then increases the amount of calcium that is absorbed. When calcium levels are high, conversion of vitamin D into its active form is decreased. Learn more about the relationship between vitamin D and the parathyroid here.
The ability to perform this conversion is also available within cells outside of the kidneys, as part of vitamin D’s function within the paracrine system. In this situation, such as with an immune response, a cell has a specific need for 1,25D. It will then pull D3 or 25(OH)D into the cell and convert it into its active form, where it can act directly within the cell to produce the desired function. More can be learned about the endocrine vs. the paracrine functions of vitamin D here.
Preventing Excessive Vitamin D Activity
A process known as 24-hydroxylation occurs to both 25(OH)D and 1,25D. The enzyme responsible for initializing this reaction for 1,25D is located in all tissues where vitamin D is active, and acts to prevent excessive vitamin D activity by terminating its effect and rendering it inactive.
The majority of 24-hydroxylation for 25(OH)D occurs in the kidneys, and results in a form of vitamin D called 24,25D, which then circulates in the blood. Not much is known about the role of 24,25D, however, some studies show that it improves fracture healing and may be better than 1,25D at repairing mineralization defects that occur from vitamin D deficiency.
Do You Have Too Much or Too Little Vitamin D?
What is your vitamin D level? Make sure you know yours is it at a level that could help prevent or reduce inflammation. Find out today! Log on to the shop (click the link below) to get your tests and see for yourself if your supplementation routine has helped you reach your target vitamin D level.
Make sure you track your results before and after, about every 6 months!
Click Here to Access the Shop Page
How can I track my Vitamin D levels?
To help you track your nutrient levels, GrassrootsHealth has created an online tracking system called myData-myAnswers. You can also track your supplemental and dietary nutrient intake to see how they impact your nutrient levels. Check it out today!